A Conversation with Ortho Montana's Dr. Jessica Hart

Dr. Jessica Hart is an orthopedic surgeon specializing in sports medicine at Ortho Montana in Bozeman, which serves patients across south-central and eastern Montana with locations in Bozeman, Billings, and Miles City, providing orthopedic care for both surgical and non-surgical treatments for the demanding physical lives Montanans lead. A former collegiate gymnast, she completed her fellowship at the University of Colorado before relocating to Montana, where she now treats everyone from high school athletes to working ranchers.
You’ve worked with some pretty high-profile teams—Colorado Avalanche, CU Football, Denver University Hockey. What brought you from that world to Montana, and what surprised you most about practicing orthopedics here?
Working with elite teams was an incredible experience, but Montana offered something that felt more sustainable and meaningful long-term—both professionally and personally. What surprised me most is how high the level of athleticism still is here. People may not be playing professionally, but they ski hard, work hard, and expect their bodies to perform at a very high level. The expectations are different, but the stakes are often just as high.
You were a collegiate gymnast before becoming an orthopedic surgeon. How did that experience shape your approach to sports medicine? Does having been an athlete yourself change how you understand what your patients are going through?
Being a gymnast taught me discipline, body awareness, and what it feels like to push through injury—sometimes wisely, sometimes not. I understand the frustration of being sidelined and the fear of not returning to the same level. That experience makes me very focused on function, not just imaging or timelines. I try to meet patients where they are emotionally, not just anatomically.
How does treating athletes in Montana compare to treating athletes at the D-1 or professional level? Are the injuries different, or just the context?
The injuries themselves are often similar—the ACL doesn’t care if you’re a pro or a high school athlete—but the context is very different. In Montana, athletes often don’t have layers of trainers, nutritionists, or recovery resources. They may also have jobs or family responsibilities that affect rehab. The treatment plans have to be more individualized and realistic.
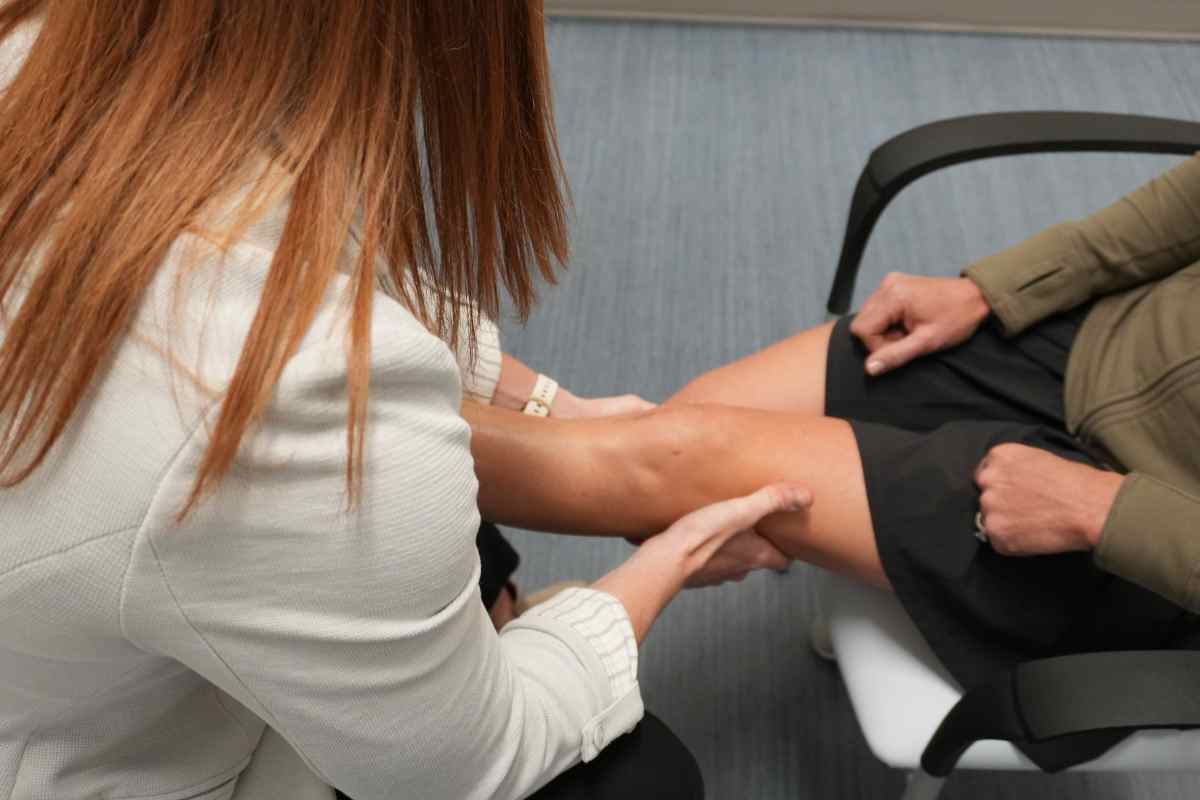
Sports medicine covers everything from weekend warriors to high school athletes to ranchers who’ve been working cattle for 40 years. How do you think about treating such different populations with such different demands on their bodies?
I start by asking one key question: What do you need your body to do? For some people, that’s returning to competitive sport. For others, it’s being able to work, ride horses, or lift grandchildren. The diagnosis might be the same, but the treatment goals—and sometimes the treatment itself—are very different.
What’s the most common misconception patients have about orthopedic injuries or recovery? What do you wish more people understood before they came to see you?
Many patients think surgery is either a quick fix—or something to fear at all costs. In reality, surgery is just one tool. Recovery is a partnership between the surgeon, the patient, and the rehab team, and the patient plays a huge role in the final outcome. I wish more people understood how much their effort, consistency, and mindset truly matter.
You did your fellowship at University of Colorado—what’s something you learned there that’s particularly relevant to practicing in Montana?
Judgment. Knowing when not to operate is just as important as knowing how to operate. Here, success means restoring strength and reliability that patients can trust—on the field, on the mountain, or on the ranch.
Are there injuries or conditions you see more frequently in Montana because of how people live and work here? What does the Montana lifestyle demand from orthopedic care?
Overuse injuries, shoulder and knee problems, and trauma related to skiing, ranch work, and outdoor recreation are very common. Montana demands durability. Orthopedic care here has to focus on longevity and resilience, not just short-term recovery.
When you’re treating someone who makes their living ranching, logging, or doing other physically demanding work, how does that change your approach to treatment and recovery?
Time away from work isn’t just inconvenient—it can be financially devastating. I think very carefully about timelines, work modifications, and whether non-operative options can safely get them back sooner. When surgery is needed, we plan rehab around real-world demands, not textbook ideals.
Orthopedic surgery remains a male-dominated field. What’s your experience been like, and has that shaped how you practice or how you connect with patients?
It’s made me adaptable and very intentional about communication. I think it’s also helped me connect with patients who may feel overlooked or intimidated in medical settings. I try to listen carefully and make sure patients feel heard and respected.
What’s the most technically challenging or interesting case you’ve worked on recently (without identifying details, of course)?
Revision shoulder surgery is always intellectually and technically challenging—especially when prior surgeries, altered anatomy, and high functional demands are involved. It’s a puzzle that requires creativity, planning, and precision.
How has orthopedic sports medicine changed in the five or ten years since you started your training? What’s exciting about where the field is headed?
We’re much more biologically focused now—thinking about tissue quality, healing environments, and longevity rather than just mechanical fixes. What’s exciting is the shift toward personalized medicine: tailoring treatments to the patient, not the protocol.
What do you do when you’re not working? How do you stay active in Montana?
I spend as much time outside as possible—skiing, hiking, working out, and keeping up with my two daughters. Montana makes it easy to stay active, but it also reminds you why protecting your body matters. Out here, movement isn’t optional—it’s part of life.












Leave a Comment Here